4 Reasons Why Physiologic Birth is Smart Policy
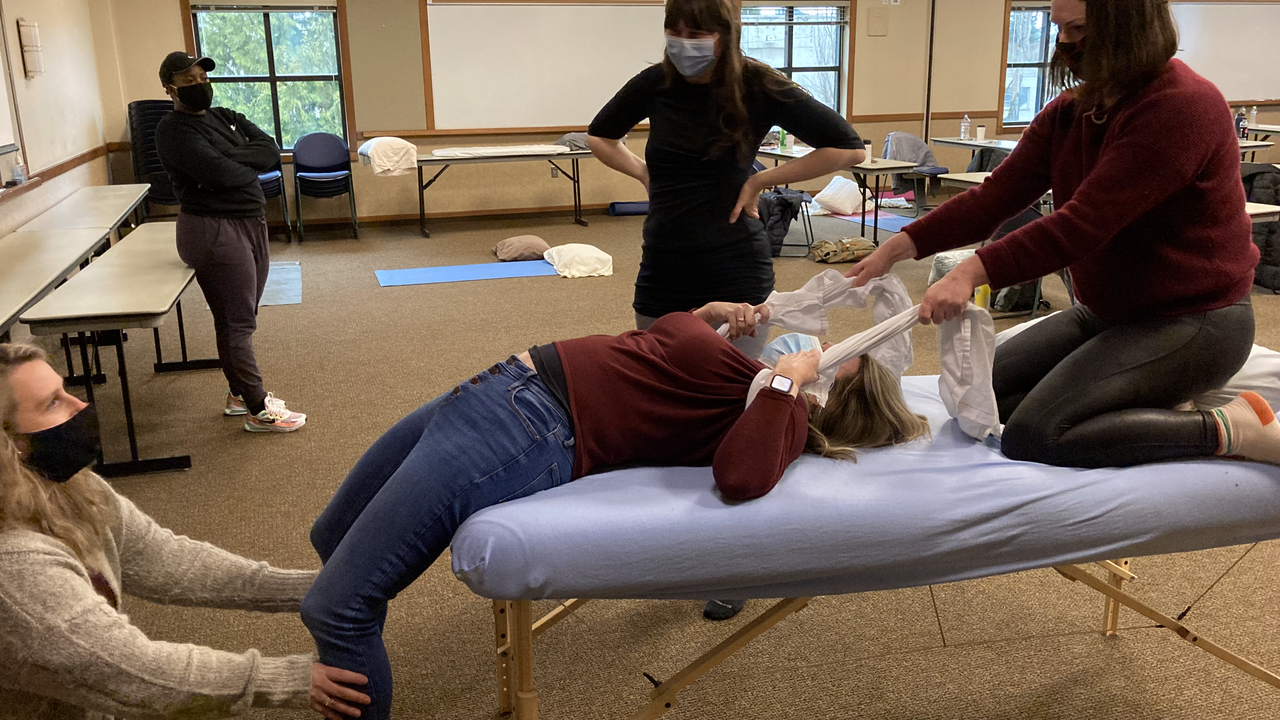
Last week, I got to go to a Spinning Babies class! You know how when you cut out sugar for a bit and then have a cookie and it tastes sooo freaking good? That's how getting to go to an in-person class again was (I know...geez Jen, get a life!). Maybe it was getting to be the student again or that it was so much new, applicable information or Kelly’s really fantastic teaching. But whatever it was, that class rocked my world. Spinning Babies takes physiologic birth and pelvic anatomy, pairs it with clues from a particular labor and delivers a number of stretches, massages, and positions to get those babies out according to whether you need to balance some part of the anatomy or make more room in the upper, mid, or lower pelvis. It’s pretty slick. Of course it isn’t going to eliminate cesarean, but it sure feels great knowing I have a few extra cards to play.
I first taught a class that included physiologic birth as a principle in 2014. I was consulting for a hospital here in Portland OR and according to the new manager, the staff hadn’t been getting much in the way of education. She wanted to do an all day crash-course in the basics. We covered some fetal monitoring, oxytocin safety and reviewed our state’s Nurse Practice Act, among other things. But if basics were what they wanted, what could be more basic than physiologic birth?
In fact, that part of the day was creatively named--wait for it--Labor Basics. We talked about intrinsic vs extrinsic value and why physiologic birth is intrinsically valuable. And we talked about why research like Listening to Mothers I, II and now III (National Partnership for Women & Families) all describe a majority of women’s preference for it. And we talked about the need to have an attitude of “why should we?” when choosing to intervene in a pregnancy or birth, instead of the prevailing “why not?” stance we seem to be moving towards.
But for all the theoretical explanations, as I’ve continued to teach the importance of physiologic birth I’m not sure I’ve changed things among my colleagues as much as I’ve hoped. So now I’m going super practical and answering the question: Why is physiologic birth smart policy? Developing a unit culture around physiologic birth can reduce nurse burnout, improve patient satisfaction, work to prevent birth trauma, and is an excellent risk management strategy.
Nurse Retention/Satisfaction (i.e. Prevent Nurse Burnout)
Burnout is affecting all healthcare workers, and perinatal nurses are no exception. When nurses feel skilled, empowered, competent, and like they can make a difference, it's shown to be highly-correlated with job-satisfaction, low-levels of burnout and high levels of resiliency (Maslach Burnout Inventory). For labor nurses, this means developing all the skills, not just fetal-monitoring or titrating pitocin. We need labor support skills that work and we need the time to be at the bedside using them. Providing education on physiologic birth, like a Spinning Babies class, to staff can bring a renewed energy. I’ve experienced it on my own unit. And we all know there’s something so satisfying about building trust with a patient and working with them to have the birth they desire. It’s rewarding, and for most perinatal nurses, we chose this field because we like birth.
Patient Satisfaction (HCAHPS/Press Ganeys/etc.)
The premise of physiologic birth is to center the patient, her knowledge and what she's experiencing. Shared decision-making is a basic premise of this relationship and is a dynamic process of collaboration between the client and the provider. It includes unbiased, evidence-based information regarding proposed interventions from the provider, and information about goals, values, preferences, and fears from the client. And we need to allow ample shared decision-making, free from coercion, to create a supportive birth environment. Any situation in which the mother feels threatened or unsupported disrupts physiologic labor. Use this as a lens to get really curious and work to eliminate language, practices (which may really just be preferences rather than evidence-based policies), or environmental elements that are disruptive and watch those HCAHPS and Press Ganeys soar!
Preventing Birth Trauma
We know birth is tremendously powerful. Powerfully transformative or powerfully devastating and traumatic. We want more of the first kind. Having embodied knowledge disregarded is a major contributor to birth trauma, so when nurses and other care providers have a deep knowledge and understanding of the physiology of birth they can validate and encourage what the birthing person is feeling as normal or right, because we actually know normal. This is the ultimate ‘when we know better, we can do better’. There are countless positions I’ve seen corrected by care providers that were actually the exact right thing physiologically! For instance, did you know bringing the knees in towards each other and the heels apart makes more room at the pelvic outlet? But over and over we ask patients to push with knees pulled apart. This is a small example, perhaps not likely in and of itself to cause trauma, but it’s easy to see how a consistent mismatch between clinical assessments and patients' sensations can accumulate to make the birth experience traumatizing.
Physiologic Birth is an Excellent Risk-Management Strategy
We get our best outcomes in birth when we don’t intervene in normal and when we intervene in a timely manner in abnormal. But what if we don’t know normal? The training we get in nursing school and in new-to-specialty orientation is variable and often focused on interventions and managing emergencies. All important stuff! But by neglecting to teach physiologic birth and the skills necessary to support it, are we really meeting the standard of care? We might not be and that’s the first risk management problem. I think we can all agree that perinatal nurses must know the physiology of birth, including the relevant maternal and fetal anatomy. And when we don’t, it opens the door to issues of inadequate consent and outcomes that lead to litigation.
Additionally, we are really force-focused in hospital birth, with the most asked question being “are her contractions adequate?”. We don’t ask the physiologic question of “why?” There are 5 P’s of Birth--passage, passenger, placenta, powers and psyche--but we are really focused on just one: power! Physiologic birth practices allow the clinician to use knowledge and skill to either simply support the process unfolding if normal or to address all of the components of a successful birth, before resorting to Oxytocin administration. And with Oxytocin misuse implicated in a large percentage of malpractice cases, it makes sense that reducing its use can also reduce adverse events and associated liability.
So there you have it! Four (more) great reasons why physiologic birth practices are not just philosophically important, but also really smart policy for inpatient birth facilities. First, physiologic birth culture increases employee retention through job satisfaction and decreased burnout. Second, it improves patient satisfaction by centering patients and shared decision-making. Third, it can offer protection from birth trauma by the validation of embodied knowledge. And lastly, by having more knowledgeable and better trained nurses at the beside, we can reduce adverse events and liability claims from misuse of oxytocin.
Let me know below: what comes to mind when you hear the term ‘physiologic birth’? What barriers do you have at your facility? I’m always happy to talk about ALL of it, so don’t be shy :)
I was really inspired to put these thoughts to paper after attending a recent Spinnning Babies course with Kelly Dungan. Please visit her website for excellent options to learn more about physiologic birth. I cannot recommend her enough and I am personally signed up for Foundations of Physiologic Birth on April 22nd and also am looking forward to BirthkeeperRN, which I suspect will convince you, if my above musings have not...I hope you’ll join me!

